Chondrocytes vs Osteocytes: Key Differences in Cellular Structure and Function
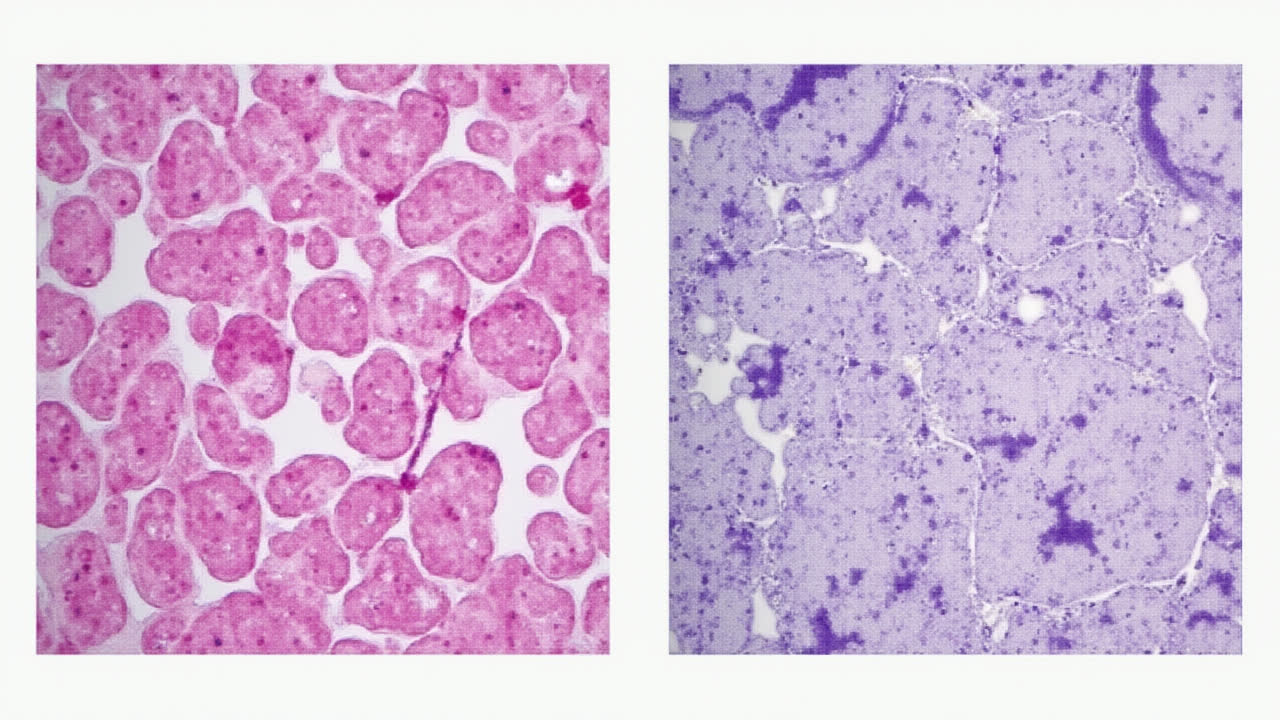
Our bodies are incredible machines, with countless specialized cells working together to keep everything functioning smoothly. When it comes to our skeletal system, two cell types play particularly crucial roles: chondrocytes and osteocytes. These microscopic workers are essential for maintaining the structure that allows us to move, protects our organs, and gives our bodies their shape.
Have you ever wondered what makes bones hard but cartilage flexible? The answer lies in these specialized cells and how they interact with their surroundings. In this article, we'll explore the fascinating differences between chondrocytes and osteocytes, their unique functions, and why understanding them matters for overall health.
Understanding Connective Tissues: The Foundation
Before diving into the specific cells, it's important to understand the bigger picture. Connective tissues are the body's internal support network, connecting and supporting other tissues throughout the body. They come in three primary types: loose connective tissue, dense connective tissue, and special connective tissue.
These remarkable tissues perform multiple functions that are essential for our survival and well-being. They repair damaged tissue, transport nutrients between tissues and organs, provide cohesion and internal support, and even store fat. In fact, you'll find connective tissues in almost every part of your body, from your bones and cartilage to adipose tissue and lymph.
What makes connective tissues so special is their composition—a combination of cells, gel-like substances, and fibers. Among these cells, chondrocytes and osteocytes stand out for their specialized roles in maintaining different parts of our skeletal system. I've always found it fascinating how these microscopic structures can have such profound effects on our overall body function and mobility.
Chondrocytes: The Cartilage Specialists
Chondrocytes are the unsung heroes of our cartilage tissue. These rounded cells are embedded within the cartilage matrix, primarily found in articular cartilages (the smooth tissue covering the ends of bones where they form joints) and intervertebral discs (the cushions between vertebrae). Though they make up only about 1% of cartilage tissue, their impact is enormous.
What exactly do chondrocytes do? Their main job is to produce and maintain the structural components of cartilage. They release specific substances that give cartilage its unique properties—both strong and flexible at the same time. This dual nature is what allows your joints to move smoothly while absorbing shock. I remember learning that without properly functioning chondrocytes, our joints would quickly wear down from the constant friction of movement.
Beyond basic maintenance, chondrocytes play crucial roles in homeostasis within articular cartilage joints, providing cushioning during movement. When tissue damage occurs, they spring into action, helping with chondral repair and responding to outside trauma. Their reconstructive nature gives them impressive healing capabilities. Additionally, these cells secrete enzymes and growth factors that regulate the extracellular matrix—the environment surrounding the cells.
Interestingly, chondrocytes don't appear out of nowhere. They develop from bone marrow mesenchymal stem cells, highlighting the interconnected nature of our body's developmental processes. This connection between different cell types reminds us that our body works as a unified system, with each component affecting others in complex ways.
Osteocytes: The Bone Guardians
Shifting our focus to bones, we encounter osteocytes—the most abundant cells in mature bone tissue, accounting for an impressive 90-95% of all bone cells in adults. Unlike their cartilage counterparts, osteocytes have a distinctive star-shaped (stellate) appearance, with cytoplasmic processes radiating outward in all directions. This unique structure allows them to connect with other osteocytes through gap junctions, forming a complex communication network throughout the bone.
Osteocytes develop from osteoblasts (bone-forming cells) and produce specific proteins such as dentin matrix protein 1 (DMP1). One of their most remarkable features is their sensitivity to mechanical forces. These cells serve as the principal sensors for mechanical loading of bone, helping the skeletal system adapt to physical stresses. When you exercise regularly, it's osteocytes that detect the increased load and signal for bone strengthening—a prime example of how our lifestyle directly influences cellular activity.
Beyond sensing mechanical strain, osteocytes regulate both local and systemic mineral homeostasis, modify the bone microenvironment, and send signals for bone formation and resorption to the bone surface. They're instrumental in the continuous process of bone remodeling, responding to even the slightest changes in bone deformation. When calcium levels in your body drop, osteocytes help remove calcium from bones to maintain proper balance.
Perhaps most impressive is the longevity of osteocytes—they can live as long as the bone itself, making them some of the longest-living cells in your body. This long lifespan allows them to maintain consistency in bone structure over time, something I find particularly fascinating when considering how our skeleton provides lifelong support.
Key Differences Between Chondrocytes and Osteocytes
| Characteristic | Chondrocytes | Osteocytes |
|---|---|---|
| Definition | Cells present in cartilage tissue | Cells present in bone tissue |
| Cell Shape | Round shape | Star shape (stellate) |
| Location | Cartilage tissue (articular cartilages, intervertebral discs) | Bone tissue (embedded in bone matrix) |
| Cell Products | Cartilage matrix, collagen, extracellular matrix | Proteins (e.g., DMP1) and soluble factors (do not secrete matrix) |
| Cell Connections | Limited direct connections between cells | Connected by GAP junctions forming a network |
| Lifespan | Shorter lifespan | Long lifespan (can live as long as bone) |
| Abundance | About 1% of cartilage tissue | 90-95% of cells in mature bone tissue |
| Primary Function | Produce and maintain cartilage structure and flexibility | Sense mechanical forces and regulate bone remodeling |
Clinical Significance: Why Understanding These Cells Matters
The differences between chondrocytes and osteocytes aren't just academic curiosities—they have real implications for human health and disease. Understanding these cells helps medical professionals develop targeted treatments for various skeletal conditions.
For instance, in osteoarthritis, the breakdown of cartilage leads to joint pain and stiffness. Researchers are exploring ways to stimulate chondrocyte activity to promote cartilage repair and regeneration. Similarly, conditions like osteoporosis involve abnormal osteocyte function, leading to decreased bone density and increased fracture risk. By targeting the signaling pathways of osteocytes, new treatments aim to improve bone strength and prevent fractures.
Sports medicine particularly benefits from knowledge about these cells. Athletes frequently experience cartilage and bone injuries, and understanding cellular responses helps determine appropriate recovery times and rehabilitation protocols. I've seen how this knowledge translates to better outcomes for patients recovering from joint injuries, allowing for more personalized treatment approaches.
Moreover, tissue engineering and regenerative medicine are revolutionary fields that leverage our understanding of chondrocytes and osteocytes. Scientists are developing scaffolds seeded with these cells to grow new cartilage and bone tissue for transplantation. This promising approach could eventually eliminate the need for artificial joint replacements and bone grafts, offering more natural and lasting solutions for patients with severe skeletal damage.
Frequently Asked Questions
How do chondrocytes and osteocytes contribute to aging and skeletal health?
As we age, both chondrocytes and osteocytes undergo functional changes that affect skeletal health. Chondrocytes show decreased proliferation and synthetic activity, leading to thinner, more fragile cartilage in joints. This contributes to the development of osteoarthritis and joint stiffness common in older adults. Meanwhile, osteocytes experience increased cell death (apoptosis) and diminished ability to sense mechanical stimuli. This reduced mechanosensitivity disrupts normal bone remodeling, often resulting in decreased bone density and increased fracture risk. Regular physical activity, calcium and vitamin D supplementation, and balanced nutrition can help maintain proper functioning of these cells throughout the aging process.
Can damaged chondrocytes or osteocytes be regenerated?
Chondrocytes and osteocytes have different regenerative capabilities. Cartilage has limited regenerative potential because chondrocytes lack direct blood supply, making natural repair difficult once damaged. However, modern therapeutic approaches like autologous chondrocyte implantation (ACI) can transplant healthy chondrocytes to repair damaged cartilage. Osteocytes, while longer-lived, can be replaced during the bone remodeling process, where old or damaged bone containing osteocytes is removed and replaced with new bone. Emerging therapies using mesenchymal stem cells show promise for regenerating both cell types, potentially revolutionizing treatment for conditions like osteoarthritis and osteoporosis.
How do lifestyle factors affect chondrocyte and osteocyte function?
Lifestyle factors significantly impact both chondrocyte and osteocyte function. Regular, moderate exercise stimulates osteocytes to signal for bone strengthening and helps maintain healthy cartilage by improving nutrient delivery to chondrocytes. Conversely, sedentary behavior can lead to weakened bones and cartilage degradation. Nutrition also plays a crucial role—calcium and vitamin D are essential for proper bone mineralization, while collagen-supporting nutrients like vitamin C benefit cartilage health. Smoking negatively affects both cell types by reducing blood flow and oxygen delivery, while excessive alcohol consumption impairs the function of bone-forming cells and disrupts calcium balance. Maintaining a healthy weight reduces mechanical stress on joints, benefiting chondrocyte longevity and function.
Conclusion
Chondrocytes and osteocytes may be microscopic, but their importance to our skeletal health can't be overstated. While both are vital cells in connective tissues, they differ significantly in location, shape, function, and longevity. Chondrocytes, with their round shape, maintain cartilage tissue flexibility and strength, primarily in joints and intervertebral discs. Meanwhile, star-shaped osteocytes oversee bone health, acting as mechanical sensors and regulators of mineral balance.
Understanding these differences isn't just academic—it has profound implications for treating skeletal disorders, developing regenerative therapies, and maintaining overall health as we age. The next time you move a joint or put weight on your bones, remember the intricate cellular ballet that makes these actions possible. Our skeletal system truly demonstrates the remarkable specialization and cooperation of cells that keep our bodies functioning throughout life.